The Peripheral Nerve is responsible for taking the commands from the brain to the muscles so that they perform movements, in addition to bringing the stimuli of pain, sensitivity, pressure and touch from the periphery to the brain, so that they can be interpreted. After a cut on the hand, the patient should immediately seek a hospital. Every cut on the hand must be urgently examined by a trained doctor.
What is a Peripheral Nerve?
The nerve is an extremely delicate structure that is shaped like a tube and has the main function of carrying nerve stimuli (electrical currents) from the brain to the extremities of the limbs and bringing them back. They work like a light cable, carrying and bringing energy and commands, which will be interpreted by the different organs.
The nerve functions as a large hollow cable filled with extensions of nerve cells. The processes that carry stimuli from the brain to the periphery are axons and those that bring them back are dendrites.
What is the Function of a Peripheral Nerve?
The nerve is responsible for taking the commands from the brain to the muscles so that they perform movements, in addition to bringing the stimuli of pain, sensitivity, pressure and touch from the periphery to the brain, so that they can be interpreted.
Nerves also carry the command for the correct functioning of blood vessels (arteries and veins), controlling their caliber and blood flow, in addition to controlling the function and growth of hair, skin and nails.
What Care Should You Take After a Cut?
Before going to a hospital, clean the wound and cover it with a clean cloth or towel. A tourniquet, belt or tourniquet should not be placed to reduce local circulation. This only increases tissue damage. When there is considerable bleeding, a compressive dressing can be applied to the wound. This pressure will stop bleeding. Also, no bleeding vessel should be clamped with forceps. Clamping will make surgical reconstruction impossible.
After a cut on the hand, the patient should immediately seek a hospital. Every cut on the hand must be urgently examined by a trained doctor. An open wound, including only the skin, has a fair amount of time to close. Generally, a cut is not sutured after six hours of evolution, as the risk of infection increases.
After an accident, the patient must stop eating and drinking. In case of urgent surgery, anesthesia will be safer if the patient is fasting.
Whenever it is suspected that a cut has caused a nerve rupture, the patient should not be anesthetized before all tests have been carried out. The infiltration of Xylocaine in the wound will cause the nerve to lose its function for a period of up to 10 hours, making it impossible to define the diagnosis.
What Does the Patient Feel With a Nerve Injury?
Initially, the patient feels loss of skin sensitivity in the region distal to the cut. She will be anesthetized there. Often the patient remains with protective sensitivity. That is, he even feels that some object causes an injury or burn to the skin, but he cannot determine precisely what it is.
He will also lose control of the muscles that are controlled by that nerve. Muscles become flaccid and functionless, which can lead to joint deformities.
Whenever there is a cut at the anatomical location of a nerve’s path and there is numbness in the skin, there is a strong suspicion of a nerve rupture. However, there are different types of injuries, which can be partial and total.
How is the Diagnosis Made?
The diagnosis of nerve damage is clinical, made by the hand surgeon when examining the patient. To determine the severity of the injury (to know if it was complete), there are specific tests.
One of them is called two-point discrimination. With normal fingertip sensitivity it is possible to differentiate the touch of two sharp objects less than 5 millimeters apart. When there is a cut and the patient cannot distinguish two points that are more than 10 millimeters apart, it is known that the nerve is completely ruptured.
Another test that can be used, especially for pediatric or difficult-to-cooperate patients, is to place the extremity in a basin of water. Normally innervated skin becomes wrinkled when exposed to water for a long time. If the innervation of this region is damaged, the skin remains smooth.
At the site of the cut, whenever there is damage to a nerve, there will be a sensation of shock when being touched, similar to a bare electrical wire. We call this the Tinel Signal.
Tests used for chronic and compressive nerve injuries, such as Electroneuromyography, are not very useful in acute trauma. The results are often confused due to the passage of some electrical discharge to the wound site and the overlapping innervation in the skin.
Is Every Peripheral Nerve Injury Treated With Surgery?
First, it is important to understand the anatomical location of the nerve. Every injury that affects the body of the neuron does not have complete recovery. Neuron bodies are located in the brain (head) or spinal cord (spine). Therefore, injuries in these places, in the vast majority of cases, leave serious, often irreversible, sequelae. On the other hand, lesions that affect the extensions of neurons (peripheral nerves) are capable of regeneration (growth). But for this recovery to be effective and organized, the external membrane that covers the nerve must be intact.
It is also important to differentiate the types of injuries. Injury that results from an open wound, such as a cut, crush, or gunshot wound, should be treated with surgery. Closed lesions, in which there is no opening in the skin, usually do not need surgery.
What is Peripheral Nerve Surgery?
In surgery, the two ends of the nerve are connected, so that the extensions of the neurons can grow in an organized way. This is an extremely delicate surgery, as the nerves are often a millimeter in diameter or less.
After a cut, the nerve works like a rubber band, that is, it shortens over time. The aim of the surgery is to remake the protective membrane of the nerve and align the extensions of the neurons, thus preventing the two parts of the tube from becoming separated.
Due to the small caliber and delicacy of the nerves, for its reconstruction we use materials and instruments made specifically for this type of surgery. They are called microsurgical materials. They are microscopes, magnifying glasses, tweezers, scissors and suture threads (these are often thinner than hairs).
How is Recovery?
The extensions of neurons have the ability to regenerate and grow after injury. Thus, whenever there is a cut in a peripheral nerve, there is an attempt to grow it back to its original location.
Once injured, the peripheral nerve will enter a period of rest for 30 days. During this period it does not grow or regenerate. After that, the extensions of the neurons will grow by an average of one millimeter per day. It will be 3 centimeters per month. Therefore, the further the injury occurs in relation to the target organ, the longer the recovery.
This recovery can be followed through the Tinel Sign. Progressively, the patient begins to feel the shock in a position further away from the injury site.
What is a Neuroma?
Neuroma is a kind of tumor that forms in the disorganized attempt of nerve growth and regeneration. It occurs when the nerve grows and does not “find” the other side of the tube (the two ends of the nerve are separated). One end becomes bulky and extremely sensitive by exposing neurons without a protective layer.
This painful swelling of the nerve tip is called a neuroma.
What are the Factors that influence the Treatment?
There are factors related to the patient, the surgery and the type of injury.
The younger the patient, the greater the ability of the nerve to regenerate, especially in children. In adults, less regeneration is observed after age 60. A clean cut, by knife or guillotine, is easier to treat when compared to crushing or pulling injuries. Systemic diseases, such as diabetes, also have a detrimental effect on regeneration. A long period between cutting and surgery is also harmful. The location of the cut also influences. Cuts on the fingers heal faster than cuts on the elbow or arm.
Changes in other tissues associated with nerve injuries, such as fractures, skin loss, or tendon injury, also alter the nerve’s recovery. Each tissue has a specific treatment and a period of regeneration and rest. So when there are several injuries at the same time, one can interfere with the healing of the other.
Another factor that we have to avoid and that has a negative effect on treatment is infection.
How is a chronic injury treated?
Any injury that is not treated in the initial phase is more difficult. Nerve damage is considered chronic after three weeks of evolution. In the first few days after the trauma, the surgeon can easily bring the ends of the nerve cables to their original position and connect them. However, after a few weeks, the ends shorten and it is no longer possible to place them against each other.
For these cases, we use a nerve graft. Nerves are taken from another location and function as bridges connecting the two ends. They are a kind of tube that allows the growth of the extensions of neurons inside.
The nerves used as a graft are less important than the injured one and their removal will not cause functional impairment. The most used is the Sural Nerve, from the lateral portion of the leg. It is only sensitive and is relatively thick and long. It is responsible for the sensitivity of a small lateral portion of the foot, and its removal is well tolerated.
Whenever possible, we use nerves from the same limb as the lesion as a graft. In the arm we used the Medial Cutaneous Nerve of the Forearm. It has similar characteristics to the Sural Nerve, being responsible for the sensitivity of the inner portion of the forearm.
There is no time limit for the recovery of sensory nerves, even after years they can be reconstructed. The motor nerves (which control muscles) must be treated within a year, after which there is a definite atrophy of the muscles. For these patients and also for cases where there is not a complete recovery after the surgery, we can do tendon transfers. They consist of using functioning tendons and muscles to replace paralyzed ones.
How is it after surgery?
It is important for the patient to be aware that recovery is slow, and can take up to a year. Often, after surgery, no change in symptoms is noticed. Improvement will only be seen weeks or months later, with the growth of the nerve and the return of sensitivity and muscle function.
Symptoms such as shock at the wound site or a burning sensation in the skin may improve soon after surgery.
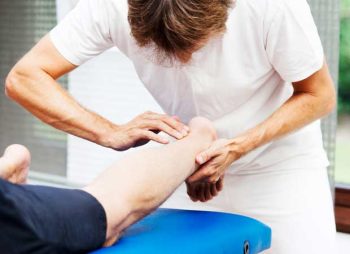
Is Physiotherapy Necessary After Surgery?
Rehabilitation after peripheral nerve surgery is primarily aimed at restoring the function of tissues that were not injured in the trauma, such as muscles, tendons and joints. Immobilization of these structures causes atrophy and stiffness that is difficult to recover.
Nerve regeneration takes a long time, but there are activities and exercises that encourage this recovery. The use of different stimuli on the anesthetized part makes the nerve recover faster.
What are the Changes for the Future?
Research carried out mainly on laboratory animals shows that certain substances and cells have the ability to stimulate faster nerve growth. Among them are growth factors, stem cells and platelet-rich plasma. These substances are present in the patient and are removed and concentrated before being used.
There have also been attempts to improve nerve grafts. Artificial tubes (absorbable or not) and natural tubes (such as veins and arteries) were tested trying to avoid a second incision for the removal of the nerve graft. Several studies have shown good results, but nothing has been superior to the classic nerve graft procedure.